Asthma Drugs by Recommended by Allergist / Immunologist
While diagnosing for asthma by an allergist/immunologist is more important, sometimes one is caught up in the middle of the night and cannot access the hospital in time for asthma diagnosis and prescription by the doctor. One might decide to take medicine or drugs to ease the congestion and pressure in the airways as he or she's rushed to the nearest hospital. This article will describe in details the drugs that can be used to work very fast and those that have to be used for a long time to get the maximum benefits.
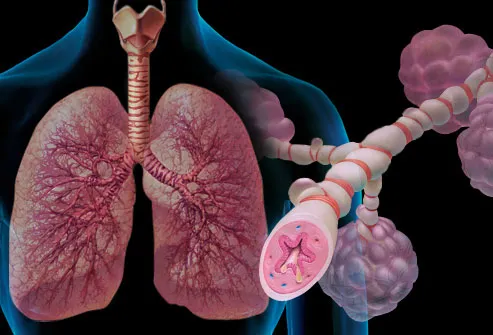
Image by Webmed
Medications
Quick-relief or rescue medications are used to quickly relax and open the airways and relieve symptoms during an asthma flare-up, or are taken before exercising if prescribed.
These include short-acting beta-agonists. This inhaled bronchodilator (brong-koh-DIE-lay-tur) medications include albuterol (ProAir HFA, Ventolin HFA, others), levalbuterol (Xopenex HFA) and pirbuterol (Maxair Autohaler).
Quick-relief medications do not take the place of controller medications. If you rely on rescue relief more than twice a week, it is time to see your allergist.
The right medications for you depend on a number of things — your age, symptoms, asthma triggers and what works best to keep your asthma under control.
Preventive, long-term control medications reduce the inflammation in your airways that leads to symptoms. Quick-relief inhalers (bronchodilators) quickly open swollen airways that are limiting breathing. In some cases, allergy medications are necessary.
Long-term asthma control medications, generally taken daily, are the cornerstone of asthma treatment. These medications keep asthma under control on a day-to-day basis and make it less likely you'll have an asthma attack. Types of long-term control medications include:
-
Inhaled corticosteroids. These anti-inflammatory drugs include fluticasone (Flonase, Flovent HFA), budesonide (Pulmicort Flexhaler, Rhinocort), flunisolide (Aerospan HFA), ciclesonide (Alvesco, Omnaris, Zetonna), beclomethasone (Qnasl, Qvar), mometasone (Asmanex) and fluticasone furoate (Arnuity Ellipta).
You may need to use these medications for several days to weeks before they reach their maximum benefit. Unlike oral corticosteroids, these corticosteroid medications have a relatively low risk of side effects and are generally safe for long-term use.
-
Leukotriene modifiers. These oral medications — including montelukast (Singulair), zafirlukast (Accolate) and zileuton (Zyflo) — help relieve asthma symptoms for up to 24 hours.
In rare cases, these medications have been linked to psychological reactions, such as agitation, aggression, hallucinations, depression and suicidal thinking. Seek medical advice right away for any unusual reaction.
-
Long-acting beta agonists. These inhaled medications, which include salmeterol (Serevent) and formoterol (Foradil, Perforomist), open the airways.
Some research shows that they may increase the risk of a severe asthma attack, so take them only in combination with an inhaled corticosteroid. And because these drugs can mask asthma deterioration, don't use them for an acute asthma attack.
- Combination inhalers. These medications — such as fluticasone-salmeterol (Advair Diskus), budesonide-formoterol (Symbicort) and formoterol-mometasone (Dulera) — contain a long-acting beta agonist along with a corticosteroid. Because these combination inhalers contain long-acting beta agonists, they may increase your risk of having a severe asthma attack.
- Theophylline. Theophylline (Theo-24, Elixophyllin, others) is a daily pill that helps keep the airways open (bronchodilator) by relaxing the muscles around the airways. It's not used as often now as in past years.
Quick-relief (rescue) medications are used as needed for rapid, short-term symptom relief during an asthma attack — or before exercise if your doctor recommends it. Types of quick-relief medications include:
-
Short-acting beta agonists. These inhaled, quick-relief bronchodilators act within minutes to rapidly ease symptoms during an asthma attack. They include albuterol (ProAir HFA, Ventolin HFA, others) and levalbuterol (Xopenex).
Short-acting beta agonists can be taken using a portable, hand-held inhaler or a nebulizer — a machine that converts asthma medications to a fine mist — so that they can be inhaled through a face mask or a mouthpiece.
- Ipratropium (Atrovent). Like other bronchodilators, ipratropium acts quickly to immediately relax your airways, making it easier to breathe. Ipratropium is mostly used for emphysema and chronic bronchitis, but it's sometimes used to treat asthma attacks.
- Oral and intravenous corticosteroids. These medications — which include prednisone and methylprednisolone — relieve airway inflammation caused by severe asthma. They can cause serious side effects when used long term, so they're used only on a short-term basis to treat severe asthma symptoms.
If you have an asthma flare-up, a quick-relief inhaler can ease your symptoms right away. But if your long-term control medications are working properly, you shouldn't need to use your quick-relief inhaler very often.
Keep a record of how many puffs you use each week. If you need to use your quick-relief inhaler more often than your doctor recommends, see your doctor. You probably need to adjust your long-term control medication.
Allergy medications may help if your asthma is triggered or worsened by allergies. These include:
- Allergy shots (immunotherapy). Over time, allergy shots gradually reduce your immune system reaction to specific allergens. You generally receive shots once a week for a few months, then once a month for a period of three to five years.
- Omalizumab (Xolair). This medication, given as an injection every two to four weeks, is specifically for people who have allergies and severe asthma. It acts by altering the immune system.
Bronchial thermoplasty
This treatment — which isn't widely available nor right for everyone — is used for severe asthma that doesn't improve with inhaled corticosteroids or other long-term asthma medications.
Generally, over the span of three outpatient visits, bronchial thermoplasty heats the insides of the airways in the lungs with an electrode, reducing the smooth muscle inside the airways. This limits the ability of the airways to tighten, making breathing easier and possibly reducing asthma attacks.
READ MORE ABOUT: VARIOUS METHODS FOR ASTHMA DIAGNOSIS
Treat by severity for better control: A stepwise approach
Your treatment should be flexible and based on changes in your symptoms, which should be assessed thoroughly each time you see your doctor. Then your doctor can adjust your treatment accordingly.
For example, if your asthma is well-controlled, your doctor may prescribe less medicine. If your asthma isn't well-controlled or is getting worse, your doctor may increase your medication and recommend more-frequent visits.
Asthma action plan
Work with your doctor to create an asthma action plan that outlines in writing when to take certain medications or when to increase or decrease the dose of your medications based on your symptoms. Also include a list of your triggers and the steps you need to take to avoid them.
Your doctor may also recommend tracking your asthma symptoms or using a peak flow meter on a regular basis to monitor how well your treatment is controlling your asthma.
Lifestyle and home remedies
Although many people with asthma rely on medications to prevent and relieve symptoms, you can do several things on your own to maintain your health and lessen the possibility of asthma attacks.
Avoid your triggers
Taking steps to reduce your exposure asthma triggers is a key part of asthma control, including:
- Use your air conditioner. Air conditioning reduces the amount of airborne pollen from trees, grasses and weeds that finds its way indoors. Air conditioning also lowers indoor humidity and can reduce your exposure to dust mites. If you don't have air conditioning, try to keep your windows closed during pollen season.
- Decontaminate your decor. Minimize dust that may worsen nighttime symptoms by replacing certain items in your bedroom. For example, encase pillows, mattresses and box springs in dustproof covers. Remove carpeting and install hardwood or linoleum flooring. Use washable curtains and blinds.
- Maintain optimal humidity. If you live in a damp climate, talk to your doctor about using a dehumidifier.
- Prevent mold spores. Clean damp areas in the bath, kitchen and around the house to keep mold spores from developing. Get rid of moldy leaves or damp firewood in the yard.
- Reduce pet dander. If you're allergic to dander, avoid pets with fur or feathers. Having pets regularly bathed or groomed also may reduce the amount of dander in your surroundings.
- Clean regularly. Clean your home at least once a week. If you're likely to stir up dust, wear a mask or have someone else do the cleaning.
- Cover your nose and mouth if it's cold out. If your asthma is worsened by cold or dry air, wearing a face mask can help.
Stay healthy
Taking care of yourself can help keep your symptoms under control, including:
-
Get regular exercise. Having asthma doesn't mean you have to be less active. Treatment can prevent asthma attacks and control symptoms during activity.
Regular exercise can strengthen your heart and lungs, which helps relieve asthma symptoms. If you exercise in cold temperatures, wear a face mask to warm the air you breathe.
- Maintain a healthy weight. Being overweight can worsen asthma symptoms, and it puts you at higher risk of other health problems.
- Control heartburn and gastroesophageal reflux disease (GERD). It's possible that the acid reflux that causes heartburn may damage lung airways and worsen asthma symptoms. If you have frequent or constant heartburn, talk to your doctor about treatment options. You may need treatment for GERD before your asthma symptoms improve.
Alternative medicine
Certain alternative treatments may help with asthma symptoms. However, keep in mind that these treatments are not a replacement for medical treatment — especially if you have severe asthma. Talk to your doctor before taking any herbs or supplements, as some may interact with medications you take.
While some alternative remedies are used for asthma, in most cases more research is needed to see how well they work and to measure the extent of possible side effects. Alternative asthma treatments include:
- Breathing exercises. These exercises may reduce the amount of medication you need to keep your asthma symptoms under control.
- Herbal and natural remedies. A few herbal and natural remedies that may help improve asthma symptoms include black seed, caffeine, choline and pycnogenol.
Ready to take the next step in mastering your arousal and Cure your Premature Ejaculation? 👇
Get Your Copy of Mastering Your ArousalUnlock lasting control and confidence in your intimate life.
Related Posts
Trending Articles
Search Now
Recent Posts
- Understanding and Controlling Involuntary Kegels (Contractions) During Sex
- Why the Transition to Sex Can Be So Challenging After Premature Ejaculation Training?
- Why Setbacks Happen: The Truth About Orgasm During Your PE Recovery Journey
- I Prematurely Ejaculated in my Girlfriend while Trying to cure my premature ejaculation using the Guide
- Have you tried this technique once you get too close to PONR
Categories
- Premature Ejaculation
- Question & Answer
- Diseases
- Drugs
- Loans
- Insurance
- Health
- Hospital
- Lifestyle
- News
- Know How
- Education
- Travel
Comments (0)
Leave a Comment